What is a DALK ?
The cornea is made of 3 main layers:
The corneal epithelium
It is the outside layer of the cornea. It protects the eyes from external aggression. It has on average 50 µm thickness and rests on the Bowman's membrane.
The corneal stroma
It is made up of collagen fibers and is on average 550 µm thick at the corneal apex. It is located between the Bowman's membrane and Descemet's membrane, between the epithelium and the endothelium. If the corneal stroma is no longer translucent, the light will pass less well through it, and the eyesight will be altered.
The corneal endothelium
It is made up of a single layer of cells that rests on the Descemet's membrane. The function of the endothelium is to pump fluid from the stroma and to evacuate it to the anterior chamber (space between the cornea and the iris). Once damaged, this layer of cells cannot be repaired.
DALK is defined as partial-thickness cornea transplant surgery that lies on selective transplantation of the corneal stroma. The patient’s original Descemet membrane and endothelium are aimed to be preserved because healthy.
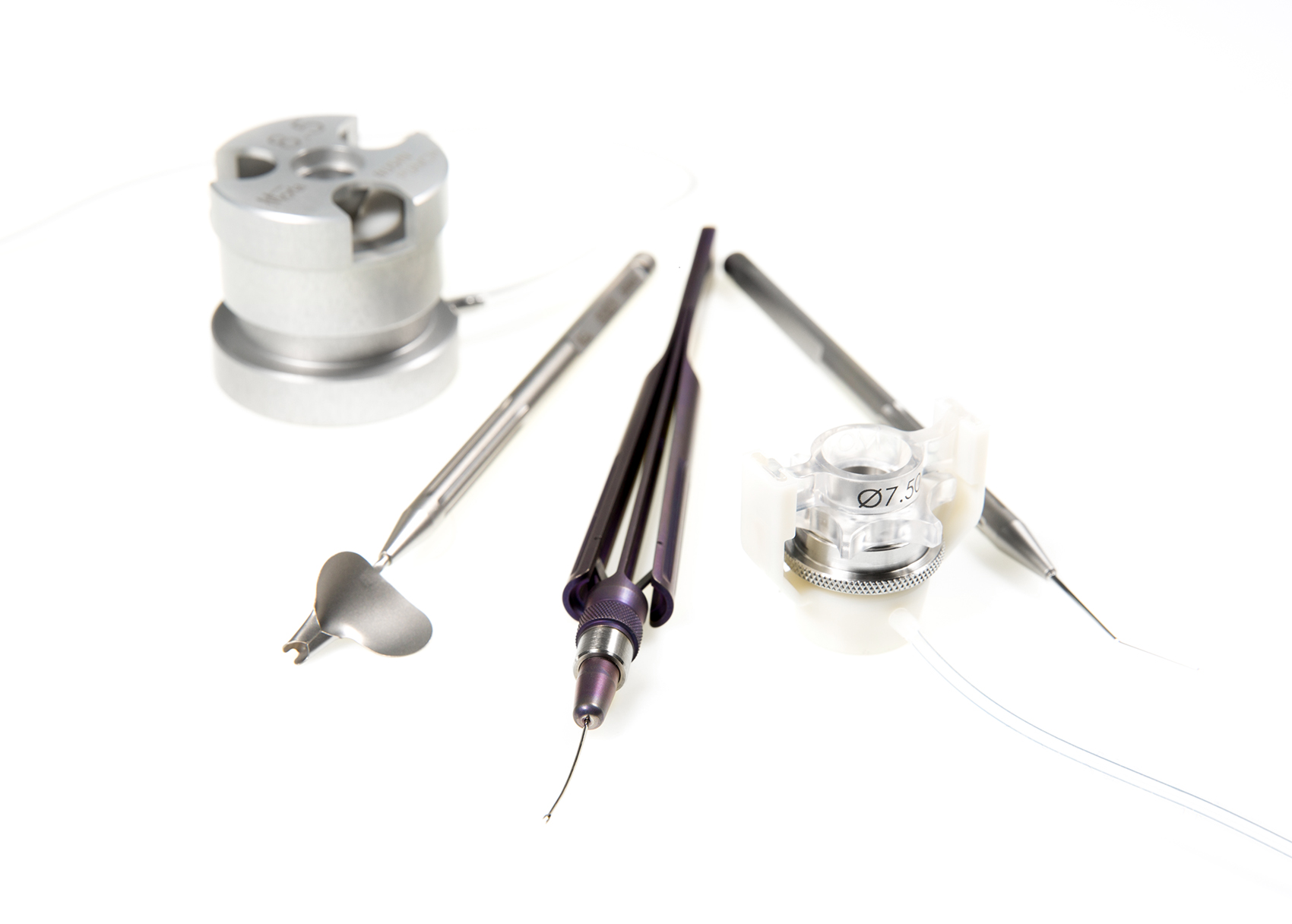
The instruments needed for Deep Anterior Lamellar Keratoplasty
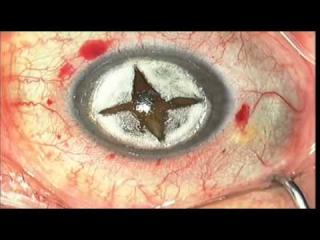
DALK requires some specific ophthalmological instruments in order to achieve success. Indeed, the surgeon starts by making a partial-thickness 360° incision into the cornea using the Moria vacuum-assisted adjustable trephine. This step is then followed by manual dissection of the anterior stroma. A corneal graft prepared from a full-thickness donor punch in which the donor endothelium-Descemet membrane complex has been removed is then placed[1].
[1] Deep Anterior Lamellar Keratoplasty (DALK) - University of Iowa HealthCare (En ligne) - https://webeye.ophth.uiowa.edu/eyeforum/tutorials/cornea-transplant-intro/3-DALK.htm
In which cases is DALK required?
Several conditions must be met before deciding if a cornea transplant can be considered.
The most common indications for DALK are:
- the presence of an anomaly in the first part of the cornea (epithelium, Bowman's membrane, or stroma) with a normal endothelial layer.
- a severe keratoconus : this condition is a progressive deformation of the cornea which affects the homogeneity of light projection on the retina.
- corneal scars : resulting from a trauma or from an infection.[2]
[2] Mayank A. Nanavaty,∗ Kanwaldeep Singh Vijjan, and Camille Yvon - Deep anterior lamellar keratoplasty: A surgeon's guide - NCBI (En ligne) - https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6276733/
What are the prerequisites for DALK?
The procedure is suited to people with a healthy endothelium who are suffering from conditions that affect the other layers of the eye, such as keratoconus or corneal scarring. In the past, this has been treated with a full-thickness transplant; DALK offers a good alternative because the patient's own endothelium is preserved, which decreases the risks of graft rejection [3].
[3] Federico Luengo-Gimeno 1, Donald T Tan, Jodhbir S Mehta - Evolution of Deep Anterior Lamellar Keratoplasty (DALK) - Pubmed.gov (En ligne) - https://pubmed.ncbi.nlm.nih.gov/21545763/
What results can be expected?
Generally speaking, the results of corneal transplants prove to be very satisfying. The cornea is an eye tissue that is not vascularized, which means that it is not connected to any veins or arteries. Hence, risks of an immune reaction or rejection are very low[4].
[4] C Cursiefen 1, F Schaub 2, B Bachmann 1 - [Update: Deep Anterior Lamellar Keratoplasty (DALK) for keratoconus. When, how and why] - National Library of Medicine - https://pubmed.ncbi.nlm.nih.gov/26832733/
Are there any risks associated with DALK?
In low-risk cases, results of a Deep Anterior Lamellar Keratoplasty are excellent. However, the more complex the person’s health condition is, the more the rejection percentage increases.
In high-risk cases, some corneal transplants may sadly fail. Not only is rejection one of the causes of failure, but there can also be some co-morbidities that might make the intervention more challenging. This is for example the case when a patient has glaucoma or eye surface alterations.
Ophthalmologists always inform patients about the prognosis of the intervention according to their health condition.
What are the postoperative instructions?
The possible side-effects after DALK surgery
The day after the intervention, surgeons check their patients’ healing. On the first postoperative day, the vision is most of the time better than before the surgery. Light sensitivity and scratchiness are common during the first week following the DALK.
Two weeks after the intervention, patients usually start to notice an improvement in their eyesight. A change in the eyeglasses is usually needed after eight weeks as there are no more visual changes after this time.
DALK advantages
DALK is a highly appreciated surgical technique for its advantages over full-thickness penetrating keratoplasty. Indeed, it shows a lower endothelial rejection rate than with penetrating keratoplasty, it reduces the risks of late endothelial cell failure and it offers a faster stabilization of the wound. Patients also appreciate the fact that they can quickly return to their physical activity and to their daily activities[6].
[6] By Vishak John, MD, Kenneth M. Goins, MD, and Natalie A. Afshari, MD
Edited by Sharon Fekrat, MD, Ingrid U. Scott, MD, MPH, and Woodford S. Van Meter, MD - American Academy of Ophthalmology (En ligne) - https://www.aao.org/eyenet/article/deep-anterior-lamellar-keratoplasty